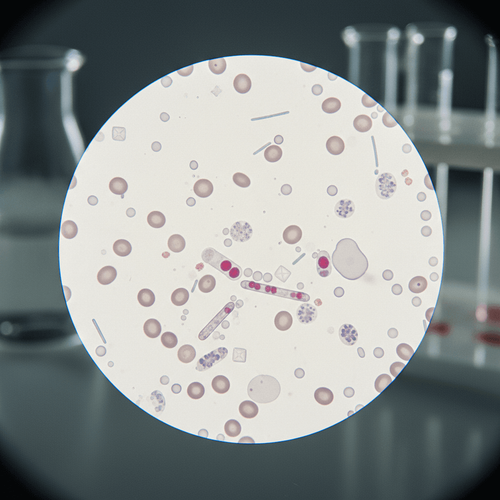
In the era of automated diagnostic testing, it's easy to overlook traditional methods. However, urine microscopy remains a vital tool for clinicians. A new guide published in Diagnostics emphasizes the enduring value of this classic test, particularly in scenarios where automated urinalysis falls short. Current practice often relies heavily on automated results, but this can lead to missed diagnoses. This article highlights specific clinical situations where urine microscopy provides critical diagnostic information.
Clinical Key Takeaways
Study Snapshot
- Focus:Identifies clinical scenarios where urine microscopy surpasses automated urinalysis.
- Key Benefit:Provides diagnostic clues, such as specific casts and dysmorphic RBCs, that alter patient management.
- Practical Advice:Offers actionable guidance for clinicians on when to request and interpret urine microscopy.
Automated urinalysis has become a mainstay in clinical laboratories, offering rapid and cost-effective results. However, relying solely on automated reports can lead to overlooking critical diagnostic information. The authors of the Diagnostics study argue that urine microscopy, when performed and interpreted correctly, remains indispensable in specific clinical situations. For frontline staff, this means understanding when to request and how to interpret microscopy results can significantly impact patient outcomes.
Top 5 Clinical Scenarios for Urine Microscopy
Here are five key clinical scenarios where urine microscopy provides superior diagnostic yield compared to automated urinalysis:
- Suspected Glomerular Disease: Dysmorphic red blood cells (RBCs) and RBC casts are highly suggestive of glomerular bleeding, indicating conditions like glomerulonephritis. Automated urinalysis may only report “hematuria” without specifying the morphology.
- Acute Kidney Injury (AKI) Evaluation: The presence of specific casts, such as muddy brown casts in acute tubular necrosis (ATN) or white blood cell (WBC) casts in acute interstitial nephritis (AIN), can pinpoint the cause of AKI. These casts are often missed by automated systems.
- Urinary Tract Infection (UTI) Diagnosis in Complex Cases: While automated urinalysis can detect pyuria, microscopy helps differentiate true infection from contamination, especially in patients with indwelling catheters or neurogenic bladder. The presence of bacteria alongside WBCs is crucial.
- Evaluation of Renal Transplant Recipients: Monitoring for casts and cellular debris is essential in renal transplant patients. Changes in these parameters can signal rejection or other complications early on, allowing for timely intervention.
- Suspected Crystal-Induced Nephropathy: Identification of specific crystals, such as uric acid or oxalate crystals, can diagnose crystal-induced nephropathy. Microscopy is superior in identifying crystal morphology and quantity compared to automated methods.
Clinical Pearls and Pitfalls
Several clinical pearls can enhance the utility of urine microscopy. First, always correlate microscopy findings with the patient's clinical context. For example, hematuria in a patient with recent strenuous exercise is less concerning than in a patient with risk factors for kidney cancer.
Second, be aware of potential pitfalls. Contamination is a common issue; proper collection techniques are essential. Additionally, delayed analysis can lead to cast dissolution and inaccurate results. As the study authors note, "Proper technique and timely analysis are critical for accurate interpretation of urine microscopy findings."
Implementing Microscopy Effectively
To effectively implement urine microscopy, laboratories should establish clear guidelines for when manual microscopy is indicated. These guidelines should be based on clinical scenarios and specific findings from automated urinalysis. Regular training for laboratory staff is essential to ensure accurate identification of urine sediment components.
Furthermore, clinicians should be educated on the value of urine microscopy and when to request it. This can be achieved through educational sessions and readily available reference materials. By integrating urine microscopy judiciously, healthcare providers can improve diagnostic accuracy and patient outcomes.
The judicious use of urine microscopy can significantly enhance diagnostic accuracy and improve patient outcomes. By understanding the specific clinical scenarios where microscopy excels, clinicians can avoid over-reliance on automated urinalysis and ensure that critical diagnostic information is not overlooked. This approach not only benefits individual patient care but also contributes to more efficient and effective healthcare delivery.
LSF-7682019790 | December 2025

How to cite this article
O'Malley L. Urine microscopy: a practical guide to when it still matters. The Life Science Feed. Published February 25, 2026. Updated February 25, 2026. Accessed February 25, 2026. https://thelifesciencefeed.com/nephrology/acute-kidney-injury/practice/urine-microscopy-a-practical-guide-to-when-it-still-matters.
Copyright and license
© 2026 The Life Science Feed. All rights reserved. Unless otherwise indicated, all content is the property of The Life Science Feed and may not be reproduced, distributed, or transmitted in any form or by any means without prior written permission.
Fact-Checking & AI Transparency
This content was produced with the assistance of AI technology and has been rigorously reviewed and verified by our human editorial team to ensure accuracy and clinical relevance.
References
- Fogazzi GB, Garigali G, Giani M. The role of urine microscopy in clinical practice. J Nephrol. 2017;30(6):727-743. doi: 10.1007/s40620-017-0419-7
- Lippi G, Plebani M. Point-of-care urine testing. Clin Chim Acta. 2018;484:167-171. doi: 10.1016/j.cca.2018.06.014
- Perazella MA, Coca SG. Urine Sediment Examination in the Diagnosis of Kidney Disease. Am J Med. 2023;136(2):139-145. doi: 10.1016/j.amjmed.2022.08.024
- James GP, Paul KL, Kissane JM. Clinical value of microscopic urinalysis. Am J Clin Pathol. 1978;70(3):349-358. doi: 10.1093/ajcp/70.3.349