The relentless march of antimicrobial resistance (AMR) continues to outpace the development of new antibiotics. We're facing a crisis where common infections are becoming untreatable, threatening to reverse decades of medical progress. The Gram-negative bacteria are particularly concerning, given their intrinsic resistance mechanisms and ability to acquire new ones with alarming speed.
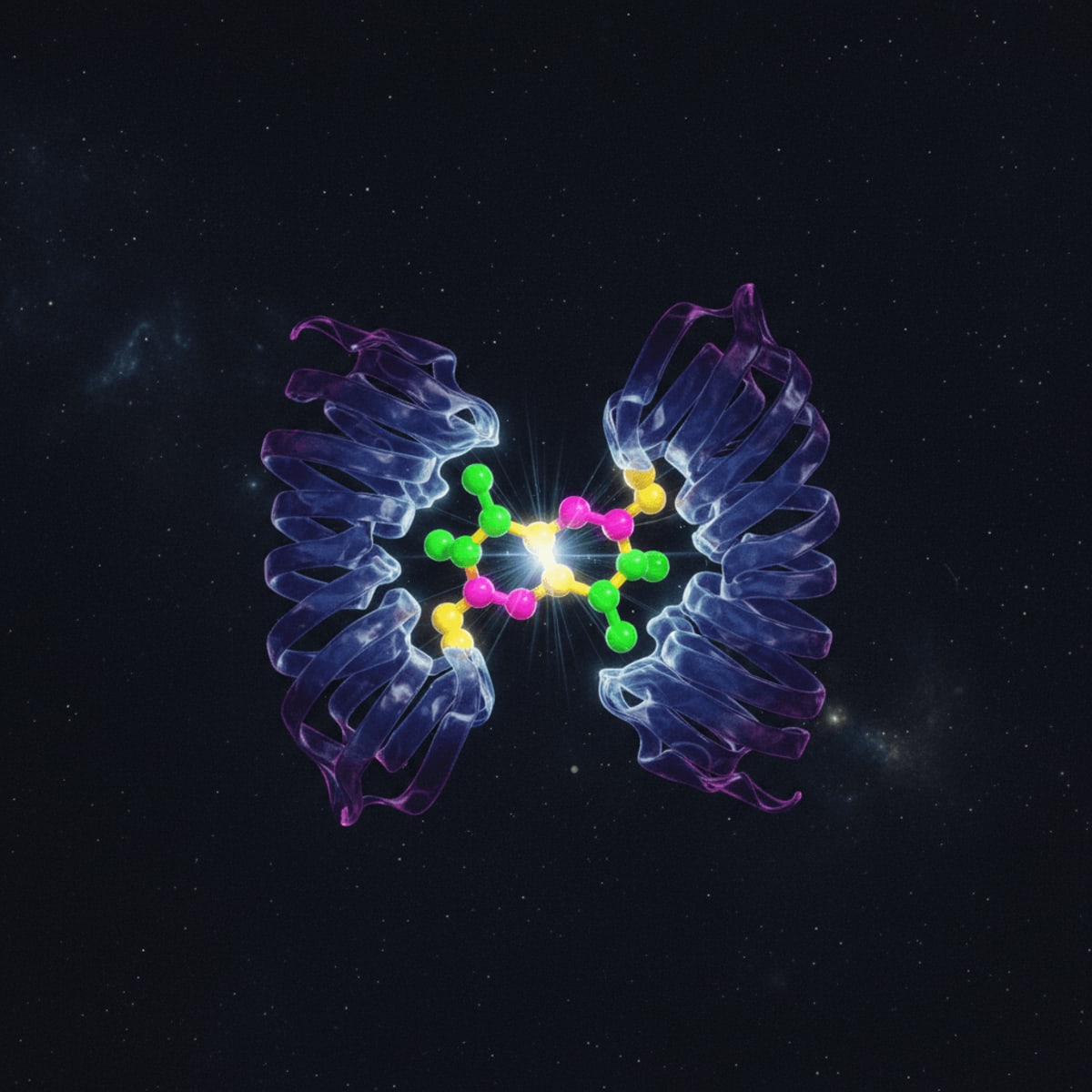
Lipophosphonoxins (LpxNs), a novel class of antibacterial compounds targeting LpxC, are generating excitement. LpxC is a vital enzyme in bacterial lipid A synthesis, a pathway absent in humans. By inhibiting LpxC, LpxNs disrupt bacterial membrane integrity, leading to cell death. The question remains whether this new class of drugs can overcome the resistance mechanisms plaguing current antibiotics.
Clinical Key Takeaways
lightbulb
- The PivotLipophosphonoxins offer a novel mechanism of action, potentially bypassing existing resistance to beta-lactams, quinolones, and other common antibiotics.
- The DataIn vitro studies demonstrate LpxNs' potent activity against a broad spectrum of Gram-negative bacteria, including multidrug-resistant strains, but clinical data remains limited.
- The ActionClinicians should monitor the development of LpxNs and related compounds as potential additions to the antimicrobial armamentarium, especially for infections where current options are failing.
The LpxC Target
Lipophosphonoxins stand out because they target LpxC enzyme, a zinc-dependent deacetylase essential for the synthesis of lipid A, a crucial component of the outer membrane of Gram-negative bacteria. This pathway is absent in humans, making LpxC an attractive target for antibacterial drug development. Inhibiting LpxC disrupts the bacterial membrane, leading to cell death. This mechanism is distinct from many existing antibiotics, which target protein synthesis, cell wall synthesis, or DNA replication. Targeting lipid A synthesis represents a potentially crucial avenue for developing new antibiotics that can circumvent existing resistance mechanisms.
Spectrum of Activity
Preclinical studies show that LpxNs exhibit broad-spectrum activity against a range of Gram-negative bacteria, including clinically relevant pathogens such as Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, and Acinetobacter baumannii. Importantly, they have demonstrated activity against multidrug-resistant strains, including carbapenem-resistant Enterobacteriaceae (CRE) and extensively drug-resistant (XDR) P. aeruginosa. The in vitro potency of LpxNs against these resistant strains is particularly encouraging, suggesting that they may offer a therapeutic option where current antibiotics are ineffective.
Overcoming Resistance
The rise of antimicrobial resistance (AMR) demands novel strategies to combat bacterial infections. Bacteria have evolved various mechanisms to resist the effects of antibiotics, including enzymatic inactivation, target modification, and efflux pumps. LpxNs' unique mechanism of action offers a potential advantage in overcoming these resistance mechanisms. Because LpxC is essential for bacterial survival, mutations that significantly alter its structure or function are likely to be detrimental to the bacteria. This contrasts with resistance mechanisms that involve acquiring new genes or modifying existing ones to bypass the drug target.
Clinical Development Challenges
While the preclinical data for LpxNs are promising, the road to clinical approval is fraught with challenges. One significant hurdle is demonstrating safety and efficacy in human clinical trials. Many promising antibacterial compounds have failed in clinical development due to toxicity, poor pharmacokinetics, or lack of efficacy. Another challenge is the potential for the development of resistance to LpxNs. Although LpxC is an essential enzyme, bacteria may still evolve resistance mechanisms over time, such as mutations that reduce drug binding or upregulation of efflux pumps. Continuous monitoring of resistance patterns will be essential to guide the clinical use of LpxNs.
Consider current guidelines. The Infectious Diseases Society of America (IDSA) and the Society for Healthcare Epidemiology of America (SHEA) published guidelines in 2016 for the management of antimicrobial resistance. These guidelines emphasize the importance of antimicrobial stewardship programs and the development of new antibiotics to combat AMR. LpxNs align with these recommendations by offering a novel approach to target Gram-negative bacteria and potentially overcome existing resistance mechanisms. However, these guidelines also stress the need for rigorous clinical trials to assess the safety and efficacy of new antibacterial agents.
Limitations
It is crucial to recognize the limitations of current data on Lipophosphonoxins. Preclinical studies, while promising, often do not translate directly to clinical success. The true efficacy of LpxNs in treating human infections remains unknown. Further research needs to address the risk of developing resistance. What mutations might arise, and how quickly? Moreover, the cost of developing and manufacturing new antibiotics is substantial, and there are concerns about the economic viability of bringing new drugs to market, particularly if their use is restricted to preserve their efficacy. This cost vs. benefit calculus must be considered to ensure that these agents reach the patients that need them most. Who will pay for this?
The emergence of Lipophosphonoxins has implications for hospital formularies and infection control protocols. If these drugs demonstrate clinical efficacy, hospitals will need to update their formularies and develop guidelines for their appropriate use. Antimicrobial stewardship programs will play a crucial role in ensuring that LpxNs are used judiciously to minimize the risk of resistance development. Given the high cost of developing new antibiotics, it is essential to address the economic barriers that may limit their availability. Policymakers and healthcare payers need to incentivize the development of new antibiotics and ensure that they are accessible to patients who need them.
Reimbursement models may need to be adjusted to reflect the value of new antibiotics in treating resistant infections. This could involve implementing value-based pricing or other innovative reimbursement strategies that reward the development of effective new drugs. Furthermore, streamlining the regulatory pathway for approving new antibiotics could help reduce the time and cost of bringing these drugs to market.
LSF-2508630488 | January 2026

How to cite this article
Sato B. Lipophosphonoxins the next generation antibiotics?. The Life Science Feed. Published March 10, 2026. Updated March 10, 2026. Accessed March 10, 2026. https://thelifesciencefeed.com/dentistry/endodontic-infections/insights/lipophosphonoxins-the-next-generation-antibiotics.
Copyright and license
© 2026 The Life Science Feed. All rights reserved. Unless otherwise indicated, all content is the property of The Life Science Feed and may not be reproduced, distributed, or transmitted in any form or by any means without prior written permission.
Fact-Checking & AI Transparency
This content was produced with the assistance of AI technology and has been rigorously reviewed and verified by our human editorial team to ensure accuracy and clinical relevance.
References
- Payne, D. J., Gwynn, M. N., Holmes, D. J., & Pompliano, D. L. (2007). Drugs for bad bugs: confronting the challenges of antibacterial discovery. Nature Reviews Drug Discovery, 6(1), 29-40.
- Powers, J. H. (2004). Antimicrobial drug development: the past, the present, and the future. Clinical Microbiology and Infection, 10(1), 23-31.
- Spellberg, B., Guidos, R. J., Gilbert, D., Bradley, J. S., Boucher, H. W., Linkin, D., ... & Bartlett, J. G. (2008). The epidemic of antibiotic-resistant infections: a call to action for the medical community. Archives of Internal Medicine, 168(13), 1357-1362.
- Liu, J., Anderson, A., Gill, C., & Tomaras, G. D. (2022). Targeting Bacterial Lipid A Synthesis: A Promising Approach to Combat Antimicrobial Resistance. Antibiotics, 11(3), 345.